159 North 3rd Street
Macclenny, Florida 32063
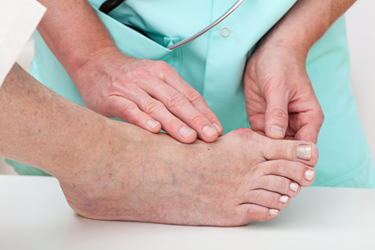 Bunions are a common foot condition that appear as a bony lump at the main joint of the big toe. They occur when the joint is pulled out of line due to the big toe being bent towards the rest of the toes. One treatment option for bunions is surgery, which is designed to straighten the big toe, allowing it to fit into shoes better. In the surgery, which will take about 30-60 minutes, your podiatrist will have a variety of options to fix the bunion, including removing the bunion, releasing the tight ligaments, realigning the bones of the big toe, or stiffening the joints and straightening out the toes. Those who are suffering from bunion pain should discuss surgery as an option with their podiatrist to see if it is right for you. If surgery is not the best option, your podiatrist will be able to provide alternative treatments.
Bunions are a common foot condition that appear as a bony lump at the main joint of the big toe. They occur when the joint is pulled out of line due to the big toe being bent towards the rest of the toes. One treatment option for bunions is surgery, which is designed to straighten the big toe, allowing it to fit into shoes better. In the surgery, which will take about 30-60 minutes, your podiatrist will have a variety of options to fix the bunion, including removing the bunion, releasing the tight ligaments, realigning the bones of the big toe, or stiffening the joints and straightening out the toes. Those who are suffering from bunion pain should discuss surgery as an option with their podiatrist to see if it is right for you. If surgery is not the best option, your podiatrist will be able to provide alternative treatments.
If you are suffering from bunions, contact Dr. John L. Coleman of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
A bunion is formed of swollen tissue or an enlargement of boney growth, usually located at the base joint of the toe that connects to the foot. The swelling occurs due to the bones in the big toe shifting inward, which impacts the other toes of the foot. This causes the area around the base of the big toe to become inflamed and painful.
Why Do Bunions Form?
Genetics – Susceptibility to bunions are often hereditary
Stress on the feet – Poorly fitted and uncomfortable footwear that places stress on feet, such as heels, can worsen existing bunions
How Are Bunions Diagnosed?
Doctors often perform two tests – blood tests and x-rays – when trying to diagnose bunions, especially in the early stages of development. Blood tests help determine if the foot pain is being caused by something else, such as arthritis, while x-rays provide a clear picture of your bone structure to your doctor.
How Are Bunions Treated?
If you have any questions, please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
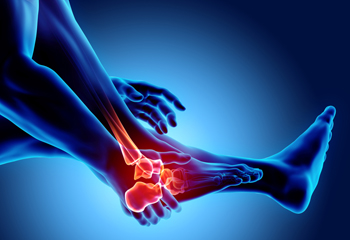 Rheumatoid arthritis (RA) is an autoimmune condition that causes the body’s immune system to attack its own healthy tissue, including the lining of joints. This leads to initial symptoms such as joint pain, swelling, stiffness, redness, warmth around the affected joints, and morning stiffness in the joints that lasts longer than 30 minutes. Typically, the smaller joints, such as those in the feet, are affected first. Over time, rheumatoid arthritis can progress, deteriorating the joint cartilage, eroding bone tissue, and restricting the affected joint’s range of motion. If you have rheumatoid arthritis that is affecting the joints of your feet and ankles, it is suggested that you seek the care of a podiatrist.
Rheumatoid arthritis (RA) is an autoimmune condition that causes the body’s immune system to attack its own healthy tissue, including the lining of joints. This leads to initial symptoms such as joint pain, swelling, stiffness, redness, warmth around the affected joints, and morning stiffness in the joints that lasts longer than 30 minutes. Typically, the smaller joints, such as those in the feet, are affected first. Over time, rheumatoid arthritis can progress, deteriorating the joint cartilage, eroding bone tissue, and restricting the affected joint’s range of motion. If you have rheumatoid arthritis that is affecting the joints of your feet and ankles, it is suggested that you seek the care of a podiatrist.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. John L. Coleman of Florida. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar fasciitis is a condition in which the ligament at the bottom of the foot, the plantar fascia, becomes inflamed due to repetitive stress or injury. It can cause heel pain, which is typically at its worst when first arising in the morning. The goal of plantar fasciitis treatment is to reduce pain and inflammation. Decreasing stress on the plantar fascia may help with this and can be achieved by resting the foot, avoiding activities that aggravate the plantar fascia, such as running or jogging, and wearing shoes or orthotics that provide more support to the arch area. Icing the foot for 15-20 minutes using an ice pack wrapped in a towel can decrease inflammation. Massaging the foot across the width of the plantar fascia can reduce pain from standing. Stretching and strengthening exercises for the foot can help prevent plantar fascia injuries in the future. If you are experiencing plantar fasciitis pain that does not get better with home treatment, it is suggested that you consult with a podiatrist.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. John L. Coleman from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
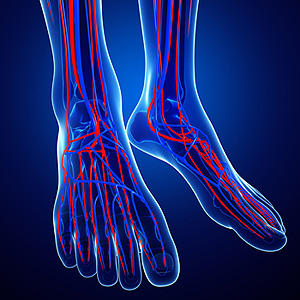 Computed tomography angiography (CTA) and magnetic resonance angiography (MRA) are two kinds of noninvasive imaging studies that can be used to visualize the blood flow in different areas of your body, including your lower limbs. A podiatrist may request that you undergo one of these imaging studies if they suspect that you might have peripheral artery disease, a condition that causes poor circulation to the lower limbs. Both of these tests require the patient to lie down on a motorized bed that moves through a scanner, which takes images of your lower legs. CTAs require the injection of an intravenous contrasting agent and the use of radiation in order to see your blood flow, while an MRA may or may not require the use of a contrasting agent, but does not use radiation. For more information about these and other tests to assess blood flow in the lower limbs, please speak with a podiatrist.
Computed tomography angiography (CTA) and magnetic resonance angiography (MRA) are two kinds of noninvasive imaging studies that can be used to visualize the blood flow in different areas of your body, including your lower limbs. A podiatrist may request that you undergo one of these imaging studies if they suspect that you might have peripheral artery disease, a condition that causes poor circulation to the lower limbs. Both of these tests require the patient to lie down on a motorized bed that moves through a scanner, which takes images of your lower legs. CTAs require the injection of an intravenous contrasting agent and the use of radiation in order to see your blood flow, while an MRA may or may not require the use of a contrasting agent, but does not use radiation. For more information about these and other tests to assess blood flow in the lower limbs, please speak with a podiatrist.
Vascular testing plays an important part in diagnosing disease like peripheral artery disease. If you have symptoms of peripheral artery disease, or diabetes, consult with Dr. John L. Coleman from Florida. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Vascular Testing?
Vascular testing checks for how well blood circulation is in the veins and arteries. This is most often done to determine and treat a patient for peripheral artery disease (PAD), stroke, and aneurysms. Podiatrists utilize vascular testing when a patient has symptoms of PAD or if they believe they might. If a patient has diabetes, a podiatrist may determine a vascular test to be prudent to check for poor blood circulation.
How Is it Conducted?
Most forms of vascular testing are non-invasive. Podiatrists will first conduct a visual inspection for any wounds, discoloration, and any abnormal signs prior to a vascular test.
The most common tests include:
These tests are safe, painless, and easy to do. Once finished, the podiatrist can then provide a diagnosis and the best course for treatment.
If you have any questions, please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.