159 North 3rd Street
Macclenny, Florida 32063

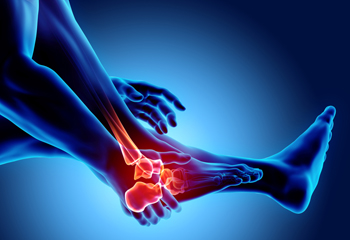 Rheumatoid arthritis is an autoimmune disease in which the body’s immune system attacks healthy joints and surrounding tissues. This leads to joint stiffness, inflammation, swelling, and pain. Rheumatoid arthritis often affects the joints of the feet and ankles. Although this is a chronic condition and does not have a cure, rheumatoid arthritis can be treated, and its symptoms can be managed. If your arthritis affects your feet and ankles, your podiatrist can help by prescribing custom orthotics, recommending exercises, and suggesting lifestyle modifications that may reduce the symptoms of rheumatoid arthritis.
Rheumatoid arthritis is an autoimmune disease in which the body’s immune system attacks healthy joints and surrounding tissues. This leads to joint stiffness, inflammation, swelling, and pain. Rheumatoid arthritis often affects the joints of the feet and ankles. Although this is a chronic condition and does not have a cure, rheumatoid arthritis can be treated, and its symptoms can be managed. If your arthritis affects your feet and ankles, your podiatrist can help by prescribing custom orthotics, recommending exercises, and suggesting lifestyle modifications that may reduce the symptoms of rheumatoid arthritis.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. John L. Coleman of Florida. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Rheumatoid Arthritis is a chronic progressive disease that attacks several joints throughout the body. It is an autoimmune disease in which the body’s immune system mistakenly attacks the joints. As a result, the tissue inside the joints, called synovium, starts to thicken and causes pain around the joints. The synovium is responsible for creating a fluid that lubricates the joints to help them move. Approximately 1.5 million people in the United States have Rheumatoid Arthritis. Women are almost three times as likely to have RA compared to men, and it’s disease usually begins between the ages of 30 and 60. People who have a genetic history of RA are more likely to develop the disease.
Symptoms of RA may include the following sensations in the joints: pain, tenderness, swelling, redness, warmth, stiffness, and loss of range. Swollen joints are a very common symptom for those with the disease. At times, it may be minimal, but it may also be very apparent. Another typical symptom is joint stiffness. Doctors will often use the direction of morning stiffness to measure the severity of a patient’s joint inflammation. Other RA symptoms include limping, anemia, fever, and fatigue.
To diagnose RA, your podiatrist will typically request x-rays to see how much damage there is in the joints. Blood tests may also be performed to show if there are any signs of anemia, or antibodies such as the rheumatoid factor. If you have previously been diagnosed with RA, you should know the disease may spread to your feet and ankles.
There are many non-surgical options that can be used to treat this ailment. Some of these options include physical therapy, foot massages, orthotics, bracing, supportive shoes, and steroid injections. Physical therapy is useful because it will help stretch and strengthen the joints in both the foot and ankle to improve joint function. Massages can help improve blood circulation which will be good for the feet. Choosing proper footwear will allow you to walk with comfortability if you are a sufferer from RA. Lastly, bracing will help stabilize the foot joints, limit deformities and decrease pain.
In severe cases, surgery may be a treatment option that should be considered. For those who cannot walk without experiencing pain and those whose deformities can not be managed with braces, surgery should be considered. Your podiatrist will recommend surgery if he or she believes it will improve your foot biomechanics.
The Achilles tendon is a collection of fibrous tissues that connect the heel bone to the calf muscles. This tendon is responsible for our ability to walk, run, and jump, but it is very vulnerable to injury from athletic activities that put excess strain on the tendon. The three most common types of Achilles tendon injuries are an Achilles tendon tear, an Achilles tendon rupture, and Achilles tendonitis. An Achilles tendon tear, in which the tendon tears slightly, is characterized by intense pain, swelling, and difficulty moving the affected ankle. An Achilles tendon rupture, in which the tendon tears completely, may make a popping or snapping sound at the time of injury, cause severe pain, and make walking extremely difficult. Achilles tendonitis is an inflammation of the Achilles tendon. It usually causes burning pain in the calf and heel that intensifies during physical activity. If you have injured your Achilles tendon, it is suggested that you seek the care of a podiatrist.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Dr. John L. Coleman of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
Rupture Symptoms
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
The Achilles tendon is the largest tendon in the body; it is a tough band of fibrous tissue that stretches from the bones of the heel to the calf muscles. This tendon is what allows us to stand on our toes while running, walking, or jumping, it is common for this tendon to become injured. In severe cases, the Achilles tendon may become partially torn or completely ruptured. However, this tendon is susceptible to injury because of its limited blood supply and the high level of tension it endures.
The people who are more likely to suffer from Achilles tendon injuries are athletes who partake in activities that require them to speed up, slow down, or pivot. Consequently, athletes who engage in running, gymnastics, dance, football, baseball, basketball, or tennis are more likely to suffer from Achilles tendon injuries. Additionally, there are other factors that may make you more prone to this injury. People who wear high heels, have flat feet, tight leg muscles or tendons, or take medicines called glucocorticoids are more likely to have Achilles tendon injuries.
A common symptom of an Achilles tendon injury is pain above the heel that is felt when you stand on your toes. However, if the tendon is ruptured, the pain will be severe, and the area may become swollen and stiff. Other symptoms may be reduced strength in the lower ankle or leg area, and reduced range of motion in the ankle. When the Achilles tendon tears, there is usually a popping sound that occurs along with it. People who have acute tears or ruptures may find walking and standing to be difficult.
If you suspect you have injured your Achilles tendon, you should see your podiatrist to have a physical examination. Your podiatrist will likely conduct a series of tests to diagnose your injury including a “calf-squeeze” test. Calf squeeze tests are performed by first squeezing the calf muscle on the healthy leg. This will pull on the tendon and consequently cause the foot to move. Afterward, the same test will be performed on the injured leg. If the tendon is torn, the foot won’t move because the calf muscle won’t be connected to the foot.
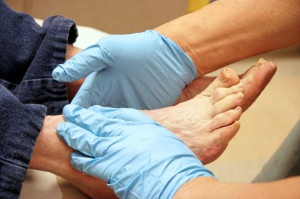 Diabetes is a disease that affects your blood sugar - so how can this condition affect the feet, too? The prolonged episodes of high blood sugar that are characteristic of diabetes often cause damage to the blood vessels throughout your body, including those that supply your lower limbs. Poor blood flow to the feet can lead to complications such as poorly healing wounds and a loss of sensation. Diabetes is associated with multiple conditions that affect the feet, including diabetic neuropathy, Charcot foot, peripheral artery disease, and gangrene. Signs of diabetes affecting the feet include swelling, tingling, numbness, weakness, skin discoloration, and foot wounds, among many others. If you have diabetes, it is suggested that you are under the care of a podiatrist, who can help you manage any foot-related symptoms.
Diabetes is a disease that affects your blood sugar - so how can this condition affect the feet, too? The prolonged episodes of high blood sugar that are characteristic of diabetes often cause damage to the blood vessels throughout your body, including those that supply your lower limbs. Poor blood flow to the feet can lead to complications such as poorly healing wounds and a loss of sensation. Diabetes is associated with multiple conditions that affect the feet, including diabetic neuropathy, Charcot foot, peripheral artery disease, and gangrene. Signs of diabetes affecting the feet include swelling, tingling, numbness, weakness, skin discoloration, and foot wounds, among many others. If you have diabetes, it is suggested that you are under the care of a podiatrist, who can help you manage any foot-related symptoms.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. John L. Coleman from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Diabetes affects millions of people every year. Blood vessels located all over the body are damaged due to diabetes—even the blood vessels of the feet. Neuropathy, or nerve damage, can result from slower blood flow in the legs and feet. In diabetic patients, neuropathy is very important to monitor, as diabetics are at risk for developing ulcers.
Always washing and thoroughly drying the feet are pertinent parts of diabetic foot care. There should be a focus on cleaning between the toes. Even if no pain is felt, the entire foot should be examined for redness and sores. Neuropathy can often mask the pain of sores and ulcers and can cause these conditions to be overlooked. Use a mirror to examine the underside of your feet if needed. It is recommended that diabetics wear well-fitting socks.
Patients with diabetes should have their doctor monitor their blood levels because blood sugar levels play a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised. It is very important to keep your blood sugar levels in the normal range, which can be determined by your physician. There are medications that may be prescribed to help with any neuropathy experienced by the diabetic patient. It is also advisable to visit a podiatrist if one is experiencing any conditions involving the feet, such as ingrown toenails, which in more severe cases can cause infection.
Diabetic feet must be inspected daily. Diabetic foot care at home is possible if a patient is provided with instructions from their podiatrist. Patients can relieve dry heels with creams or ointments. Suspected wounds should warrant an immediate call to the podiatrist. Gangrene is a serious problem for diabetics and can lead to sepsis and amputation in its worst cases. Early treatment and daily inspection of diabetic feet are keys to staying healthy.
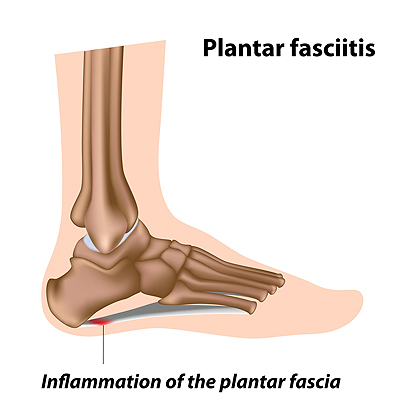 Plantar fasciitis is a condition in which the plantar fascia, a ligament that runs along the bottom of the foot, becomes injured, inflamed, and painful. Plantar fasciitis has a variety of causes, including spending too much time on your feet, engaging in high-impact repetitive activities like running, and wearing improper shoes that do not adequately support the foot. Plantar fasciitis can be treated conservatively by taking nonsteroidal anti-inflammatory medications to manage pain, stretching the feet each day, resting the feet regularly, massaging the feet, and wearing comfortable, supportive shoes. If you have plantar fasciitis, it is recommended that you see a podiatrist for treatment.
Plantar fasciitis is a condition in which the plantar fascia, a ligament that runs along the bottom of the foot, becomes injured, inflamed, and painful. Plantar fasciitis has a variety of causes, including spending too much time on your feet, engaging in high-impact repetitive activities like running, and wearing improper shoes that do not adequately support the foot. Plantar fasciitis can be treated conservatively by taking nonsteroidal anti-inflammatory medications to manage pain, stretching the feet each day, resting the feet regularly, massaging the feet, and wearing comfortable, supportive shoes. If you have plantar fasciitis, it is recommended that you see a podiatrist for treatment.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Dr. John L. Coleman from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
How Can It Be Treated?
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
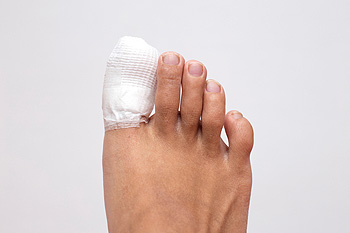 Stubbing your toe into a piece of furniture or dropping a heavy object on it are common ways to get a toe broken. It is often immediately noticed, and symptoms can include bruising, swelling, and difficulty walking. Minor fractures are treated by using the buddy taping method, which is accomplished by taping the affected toe to the toe next to it. An X-ray is generally performed to determine the severity of the broken toe, and it often takes approximately six to eight weeks to heal. If the break is severe, the bone may need to be pushed back into place, or surgery may be necessary for proper healing. If you have broken your toe, please speak with a podiatrist as soon as possible.
Stubbing your toe into a piece of furniture or dropping a heavy object on it are common ways to get a toe broken. It is often immediately noticed, and symptoms can include bruising, swelling, and difficulty walking. Minor fractures are treated by using the buddy taping method, which is accomplished by taping the affected toe to the toe next to it. An X-ray is generally performed to determine the severity of the broken toe, and it often takes approximately six to eight weeks to heal. If the break is severe, the bone may need to be pushed back into place, or surgery may be necessary for proper healing. If you have broken your toe, please speak with a podiatrist as soon as possible.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact Dr. John L. Coleman from Florida. Our doctor will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions please feel free to contact our office located in Macclenny, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.